Learn the warning signs and why a proper diagnosis of varicose vein disease is so important. Do you get cramps in your legs overnight or have restless legs? Are your legs often itchy for no apparent reason? The cause of...


Learn the warning signs and why a proper diagnosis of varicose vein disease is so important. Do you get cramps in your legs overnight or have restless legs? Are your legs often itchy for no apparent reason? The cause of...

Fluctuating hormone levels caused by pregnancy, birth control pills, hormonal treatments, and aging, can play havoc with vein health. Hormonal imbalances of progesterone and estrogen can lead to many physical problems, including the development or worsening of varicose veins. Can...
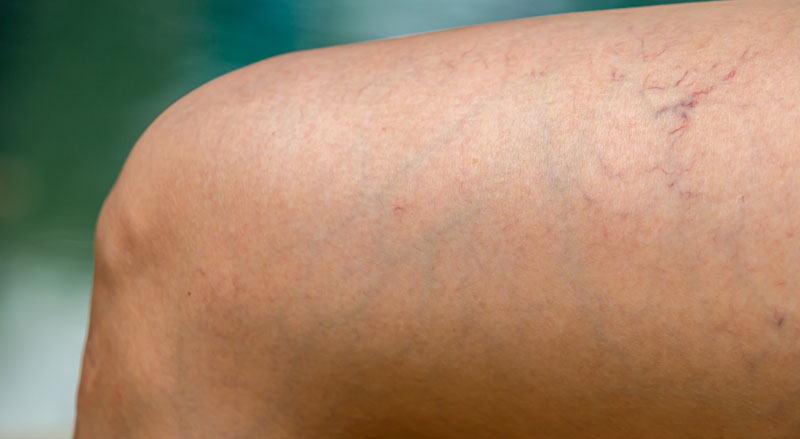
Most people know the difference between spider veins and varicose veins. But what about spider veins vs. reticular veins? What’s the difference? Veins are the structures that bring blood up from your legs and back to your heart. Three major...

Don’t think that varicose veins are just a woman’s problem. They’re a guy thing too. When it comes to varicose veins in men—here’s what you should know.
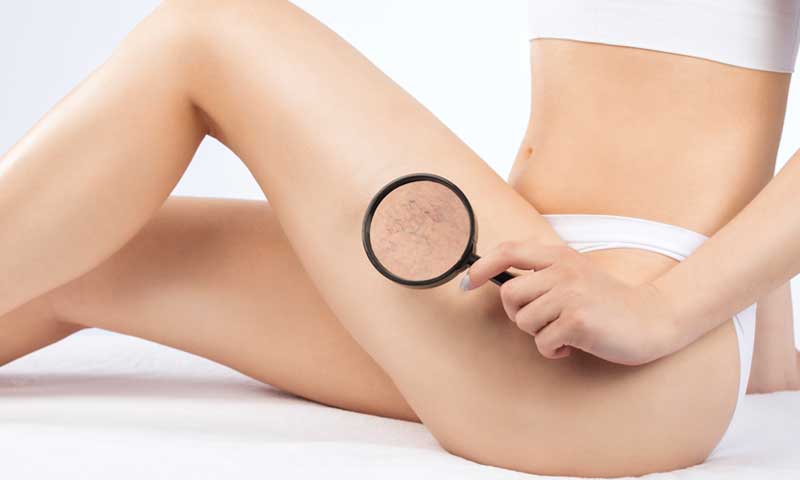
You’ve seen them before. And now you’re seeing them again! Those pesky, unattractive spider veins. Perhaps you originally had them around your ankles or on your thighs and you sought treatment. Now they seem to have reappeared, and you’re asking,...

Many people with varicose veins wonder if genetics played a role in their development—or if it destines them to get varicose veins if a parent has them. Is the answer all in your genes? And if it’s true that genetics...