Learn the warning signs and why a proper diagnosis of varicose vein disease is so important. Do you get cramps in your legs overnight or have restless legs? Are your legs often itchy for no apparent reason? The cause of...


Learn the warning signs and why a proper diagnosis of varicose vein disease is so important. Do you get cramps in your legs overnight or have restless legs? Are your legs often itchy for no apparent reason? The cause of...
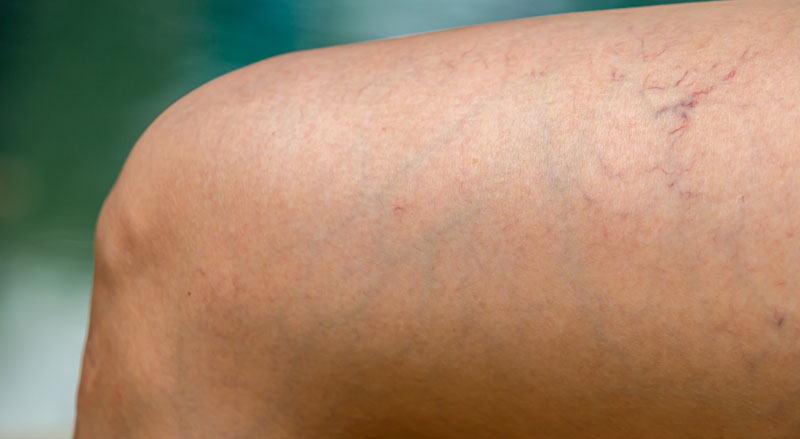
Most people know the difference between spider veins and varicose veins. But what about spider veins vs. reticular veins? What’s the difference? Veins are the structures that bring blood up from your legs and back to your heart. Three major...
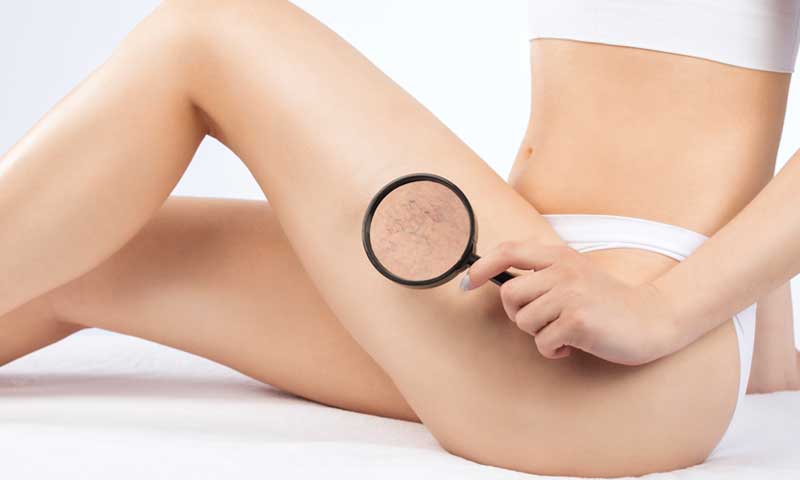
You’ve seen them before. And now you’re seeing them again! Those pesky, unattractive spider veins. Perhaps you originally had them around your ankles or on your thighs and you sought treatment. Now they seem to have reappeared, and you’re asking,...
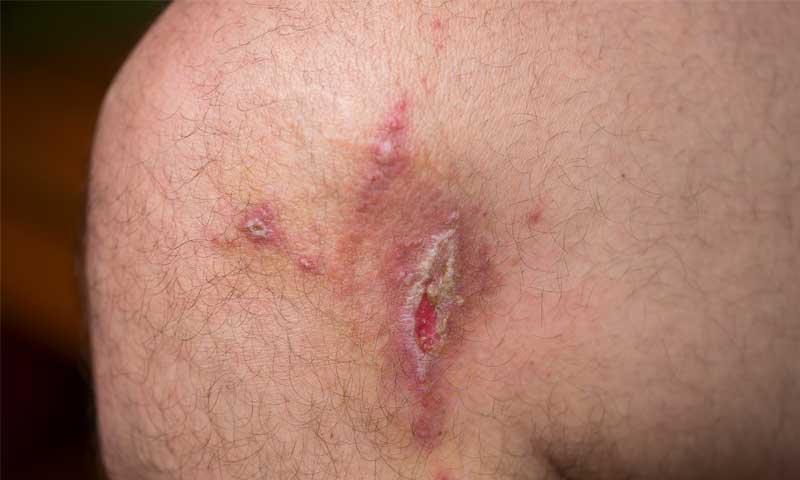
This blog covers the first signs of leg ulcers and both medical and at-home treatments. We’ll discuss why it’s important to examine the underlying causes and how to reduce and prevent their frequency. An ulcer is an open sore on...
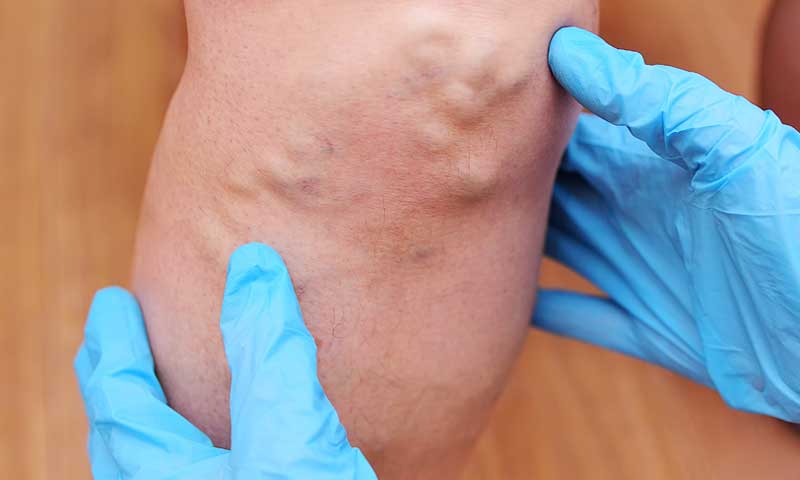
This blog covers the basics of venous insufficiency a precursor for chronic vein insufficiency( CVI). It also goes into detail about the symptoms, causes and common treatments of CVI. Over 40% of people in the United States have chronic venous...

A product of venous insufficiency, venous ulcers are a painful and stressful health issue. Managing this condition means making lifestyle changes.