
Jun 17, 2024 | General Health, Skin Conditions, Skincare
The sun’s rays play a vital role in sustaining life on Earth by providing essential warmth and light.
However, excessive exposure can have detrimental effects on our skin. Finding a balance allows us to enjoy the sun’s benefits while minimizing risks.
While some changes, such as freckles or wrinkles, may be merely cosmetic, others, like changes in color or the appearance of unusual marks, could indicate a deeper problem, such as the early stages of skin cancer.

Understanding the potential dangers of the sun is the first step in skin protection.
It’s important to safeguard ourselves, especially as environmental changes have reduced the ozone layer’s ability to block UV rays.
To stay safe in the sun, enjoy it in moderation. Limit direct exposure without sunscreen to 10-15 minutes per day.

Protective Measures for Healthy Skin
Sunscreen Is Your Daily Shield
It is essential to apply sunscreen with a minimum SPF of 30 to deflect and absorb UV rays effectively.
Choose a sunscreen formula that suits your skin type and activity level. There are mattifying options for oily skin and water-resistant types for intense exercise.
Apply the sunscreen at least 15 minutes before sun exposure and reapply it every two hours or after swimming or sweating.
Don’t Forget Your Lips

Lips are often overlooked but are highly susceptible to sunburn. Apply a protective lip balm every hour when outdoors.
Shield Your Eyes
The sun can damage your eyes and lead to cataracts.
Protect your eyes and prevent wrinkles like crow’s feet with sunglasses that offer 100% UV ray protection.
Wear a Big Hat

You don’t have to save your big, floppy wide-brimmed hat just for the Kentucky Derby!
You can wear it on the days you anticipate facing prolonged sun exposure.
A wide-brimmed hat is a stylish shade source, protecting your face, ears, and neck.
Choose UPF Clothing
UPF clothing, like sunscreen, provides different levels of protection.
This type of clothing is designed with a special coating that absorbs UVA and UVB rays.
Additionally, darker, tightly woven fabrics offer more comprehensive protection overall.
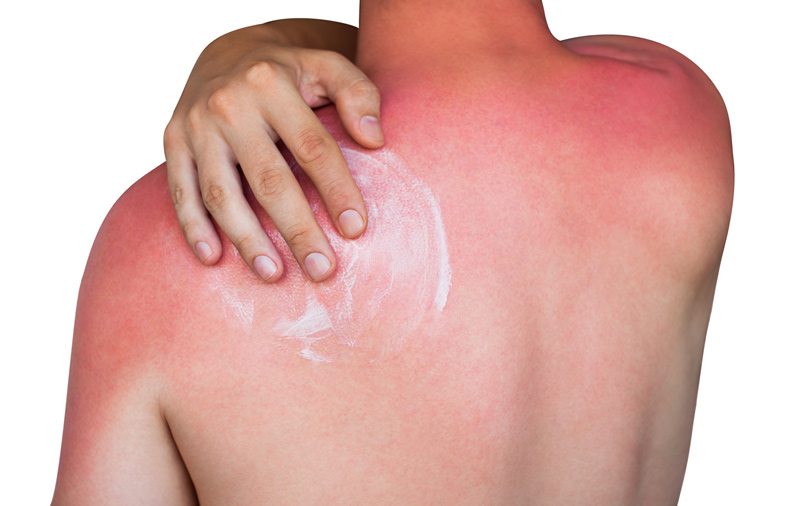
Sun Damage: Reversal and Care
Regular sunscreen use, moisturizing, exfoliation, and staying hydrated can help heal the skin.
If you notice any unusual marks or experience blistering, it’s important to seek medical attention right away.
Early intervention plays a crucial role in treating many symptoms of skin damage.

Sun Exposure and Damage: Q & A
Question: “How long can I safely be exposed to the sun, without sunscreen?”
Answer: It’s difficult to say. In the past, the ozone layer helped protect us by blocking harmful UV rays.
Over the years, the ozone layer has decreased due to air pollution and other environmental factors.
The American Skin Association states that we need to protect ourselves better as time passes and our ozone layer continues to diminish.
Brief periods can be beneficial but limiting unprotected exposure to a maximum of 15 minutes daily is wise.
Question: “When do I need to wear sunscreen?”
Answer: Every day, regardless of the season or weather. Even on cloudy days, UV rays penetrate the clouds.
Question: “Can sun damage be reversed or stopped?”
Answer: With diligent sun protection and skincare, further damage can be halted, and existing damage potentially reversed.

You need to ensure your skin’s protection while enjoying the sun’s warmth.
Sun protection, adequate hydration, and a proper skincare regimen all play a critical role in mitigating the potential risks of sun exposure.
Remember: finding balance is essential. Embrace the sun’s gifts responsibly to enjoy its benefits for years to come.
May 28, 2024 | General Health, Prevention of Vein Conditions, Vein Care, Vein Health, Vein Treatments
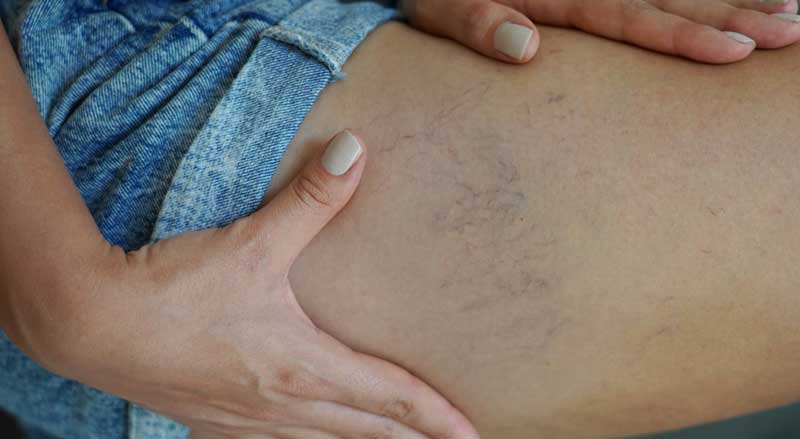
Spider veins are small veins that appear in clusters, resembling spiderwebs or tree branches.
While spider veins are not a medical concern, many individuals treat them for cosmetic reasons.
Are you wondering why you are suddenly seeing spider veins? Find the answers here.
About Spider Veins
Spider veins typically appear in clusters near the skin’s surface, commonly on the ankles, thighs, calves, and sometimes on the face. These damaged blood vessels usually appear in shades of red and blue.
Some visible spider veins are considered normal and may be expected if you have a light skin tone.
However, certain factors affecting your body may make these veins even more noticeable.
People often confuse spider veins and reticular veins. Here’s an informative article explaining the differences between the two conditions.
Reasons Veins Suddenly Become More Obvious
If spider veins suddenly appear, it’s usually because the veins are experiencing added pressure.
When veins experience more pressure, they expand in size and become more noticeable. When the pressure is reduced, the vein becomes less evident but is still under the skin.
Unfortunately, spider veins are almost always permanent—except in some instances involving pregnancy or certain medical conditions. In fact, many spider veins worsen over time.
Let’s explore the potential causes of sudden spider vein appearance and learn how to slow down the development of new veins.
Getting Older
Age is a significant factor in the appearance of spider veins for three reasons:
- As we age, we experience reduced collagen production, resulting in thinner skin and making our veins more visible.
- Gradual loss of fatty tissue makes veins more visible.
- Aging veins lose elasticity and weaken, which causes blood flow problems and results in spider veins.
Standing or Sitting for a Long Time
Prolonged periods of sitting or standing cause blood to pool in the legs. This increased pressure expands the veins and makes them more visible.
Try to change your position frequently to relieve leg pressure and encourage better circulation.
Injury to a Leg

An injury to the leg that temporarily restricts movement can cause spider veins to develop. If you can’t move your legs during recovery, keep your legs elevated.
If your leg sustains an injury, it can temporarily restrict movement, causing spider veins to develop.
If you are injured and can’t move your legs during recovery, keeping your legs elevated is essential.
Sudden Weight Gain or Obesity
Being overweight puts additional pressure on your veins. Increased pressure weakens the valves and walls of the veins, leading to the appearance of more prominent and visible veins.
Maintaining a healthy weight can aid in preventing circulation issues and stop new spider veins from forming.
Some individuals may experience weight fluctuations.
Although weight gain can alleviate pressure on the legs, it’s important to note that the veins themselves may not completely disappear.
Being Outside in Hot Weather

Hot weather can cause your veins to enlarge due to increased blood flow. Eventually, they will appear less prominent as the heat decreases.
Excessive sun exposure can also lead to the visibility of tiny veins beneath the skin.
Sunburn and UV rays cause inflammation, bringing the blood vessels closer to the skin’s surface, particularly for those with fair skin.
Additionally, prolonged sun exposure can also break down collagen in the skin, making veins more noticeable.
You can prevent this by wearing a sun-protective hat, sunglasses, and sunscreen when you spend time outside. Another alternative is to seek shade.
Vigorously Exercising
During vigorous exercise, your blood pressure naturally increases, causing your veins to expand. Understanding this process can help you feel more informed and less alarmed about the temporary visibility of your veins.

Weight-bearing exercises also pressure veins, causing them to develop a more defined appearance.
Experiencing Hormonal Changes
Puberty, birth control pills, pregnancy, and menopause can all cause veins to appear for the first time.
As hormonal shifts occur, blood flow increases, causing pressure and expansion, ultimately making veins more visible.
During pregnancy, the increase in estrogen levels and the expansion of blood volume in the body put pressure on the veins. This, combined with reduced blood flow from the legs to the pelvis, causes strain on the vein walls and the development of spider veins.
Spider veins from pregnancy can disappear on their own after several months.
Smoking and Drinking

Both drinking and smoking can cause veins to become more visible.
Alcohol increases heart rate, leading to more blood filling the veins and making them more visible. Prolonged excessive drinking can weaken veins, making them appear even more prominent.
Smoking introduces chemicals into the bloodstream, reducing oxygen and thickening the blood. This damages the vein walls, causing the veins to bulge and become more visible.
Wearing Tight Clothing
Wearing clothing that is too tight around the waist or legs can cause veins to become more visible from restricted blood flow and higher blood pressure.
It’s In Your DNA!
Genetics significantly influences the development of visible veins.
If you have close relatives with spider veins, chances are high that you will also have them.
When to See a Doctor
If a spider vein or other vein shows any of these signs, it may indicate a blood clot:
- Redness
- Warmth
- Tenderness to the touch
- Bleeding
- Discoloration around the vein accompanied by a rash or sore.
If you experience any of these symptoms, please seek medical attention immediately.
Treatments for Spider Veins
Fortunately, there are in-office treatments available that can effectively remove unwanted spider veins.
Sclerotherapy is a minimally invasive procedure that does not require anesthesia. It is recognized as the most effective treatment for eliminating spider veins and reticular veins.
Varithena™ is an incision-free treatment that usually takes less than 10 minutes. It is often used in ultrasound-guided treatments of spider veins and varicose veins.
Both Sclerotherapy and Varithena are highly effective in the treatment of spider veins.
Some veins and areas will need to be re-treated. A recurrence of the same vein is rare. Proper injection technique and patient compliance with post-treatment instructions will ensure the best results.
Here’s why some people ask if spider veins come back after treatment.
Read more about treating and preventing spider veins on the ankles.
Feel free to contact The New Jersey Vein and Vascular Center in Randolph, NJ to take the first step towards a healthier you with a vein screening and personalized treatment plan.

May 24, 2024 | General Health, Prevention of Vein Conditions, Vein Care, Vein Health, Vein Treatments
Do your legs feel achy or stiff at the end of the day? Do you experience unexplained leg pain?
If you haven’t made any substantial changes to your daily routine, or if you’re getting older, circulation health could be to blame.
The good news is that doctors can easily diagnose and treat vein diseases. Read on to find six reasons to schedule a vein screening.
Why a Vein Screening is Important
Veins and their valves play a crucial role in maintaining overall health. Healthy veins efficiently pump blood upward toward the heart, while damaged veins and valves cannot work effectively, or at all.
When veins are damaged, blood can no longer move towards the heart effortlessly—instead, it pools in your legs, resulting in poor blood circulation.
Poor blood circulation can lead to serious health issues, from slower wound healing to potentially fatal blood clots, highlighting the importance of getting a vein screening to detect any potential problems early on.
Through a comprehensive screening, a skilled vein specialist can effectively identify and address a range of vein-related diseases and concerns, providing you with peace of mind about your vein health.
Schedule a Vein Screening If You Are Experiencing These Symptoms
Restless Legs

Restless leg sensations may include:
- Tingling and burning
- Creeping and crawling
- A constant urge to move your legs
Some studies have linked restless leg syndrome to vein disease. Happily, in these cases, treatment for your vein issues may also eliminate your restless leg symptoms.
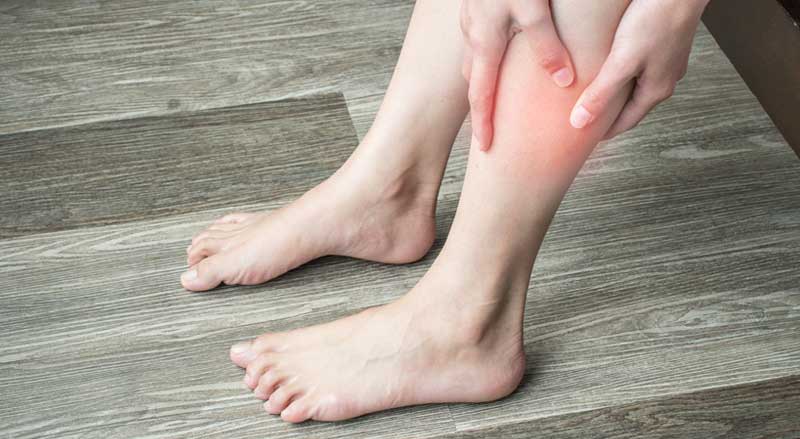
Warm or Red Areas on Your Leg or Foot
If you are experiencing throbbing pain, swelling, noticeable redness, or if the skin on one of your legs feels hot, you should consider scheduling an appointment with a vein specialist to rule out the possibility of deep vein thrombosis (DVT).
Deep vein thrombosis (DVT) is a severe health condition that involves the formation of a blood clot(s). It’s important to be aware of its seriousness and understand that it requires immediate medical attention.
If you’re a frequent traveler, take extra care. Confined spaces in planes and cars can increase the likelihood of blood clots forming in the legs. If you travel often, it’s beneficial to have periodic vein assessments to help prevent severe problems from developing during travel. Your vein doctor can advise you on measures to prevent blood clots from forming.
Read this important post about leg pain and when you should see a doctor.
Visible Veins on Your Legs
If you see spider or varicose veins on your leg, you may have a vein disease that would benefit from treatment. A vein screening will let you know the health status of your veins.
Leg Cramping or Charley Horses
Leg cramping is a common sign of poor circulation. Impaired circulation prevents the body from effectively delivering oxygen to muscle tissues in a timely manner, resulting in stiff and cramping muscles.
If you have Chronic Venous Insufficiency (CVI), you may experience cramping in your calf or feet at night as well as after sitting for an extended period during the day.
Heavy, Weak, or Tired Legs
If your legs often feel heavy, weak, or tired, it can be a sign of impaired vein function in your legs.
Swollen Feet and Ankles
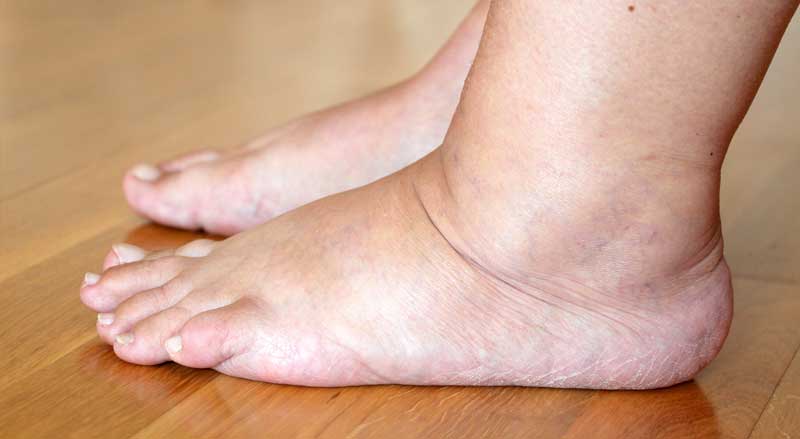
CVI can cause blood to pool, which results in the feet and ankles swelling. This swelling usually worsens as the day goes on.
Additional Symptoms
The following symptoms are additional reasons to undergo a vein screening.
- Throbbing, itching, burning legs
- Skin discoloration
- A feeling of achiness
- Cold legs
- Numb legs
- Leg discomfort when sitting or standing
- A leg ulcer that has trouble healing
Here’s additional information about warning signs and diagnosing and treating vein disease.
Family History
Did you know that vein disease is hereditary?
If you have a close family member with varicose veins, or there’s a history of blood clots in your family, you are at greater risk for developing vein disease.
Over The Age of 50
Venous insufficiency problems can develop in people as young as their 30s and 40s.
However, most people with vein disease are older than 50. This is because age usually narrows and weakens veins and valves, leading to spider veins, varicose veins, and circulatory issues.
Sedentary Lifestyle or Standing For Long Periods
Living a sedentary lifestyle has been proven to have negative effects on your health. Health experts recommend walking daily to help combat weight gain, reduce anxiety, and prevent vein disease.
On the other hand, spending prolonged periods standing at work can increase the risk of developing vein problems due to blood pooling in the legs caused by gravity.

Overweight
When a person is overweight, there is increased pressure on their veins, especially those in the lower extremities, which can cause damage.
The extra weight further stresses the body’s circulatory system, causing veins to work harder to ensure good flow. This extra work can also damage veins.
A Vein Screening is Easy
At NJVVC, we offer free Varicose vein screenings.
We welcome you to contact us with any questions about vein disease, symptoms, appointments for screening, diagnosis, or treatment.

Jul 27, 2017 | News
What is Restless Leg Syndrome?
Restless Leg Syndrome (RLS), also known as Willis-Ekbom Disease, is a neurological disorder characterized by its overwhelmingly unpleasant urges to move the legs while at rest.

What are the symptoms of Restless Leg Syndrome (RLS)?
Restless Leg Syndrome (RLS) is characterized by its overpoweringly desire to move the legs, particularly while at rest. RLS usually causes leg pain in the evening and night. A common characteristic of RLS is that, in the early morning, legs are typically symptom-free, allowing for a period of better sleep.
Who suffers from Restless Leg Syndrome (RLS)?
While RLS affects about one in ten American adults, it affects almost twice as many women than men.
Is Restless Leg Syndrome (RLS) hereditary?
RLS is not always hereditary, but genetic links have been found in some cases. RLS does seem to run in some families, but not all.

What triggers Restless Leg Syndrome (RLS)?
RLS is most commonly triggered by periods of inactivity. While RLS symptoms seem most prominent at night, the symptoms can appear at any time throughout the day when the legs are inactive. This includes sitting in theaters, on long flights or car trips, or even while relaxing at home.

Are there treatments for Restless Leg Syndrome (RLS)?
Yes! There are a variety of treatment options for dealing with RLS. First, treatment will be directed towards any known underlying illnesses. Prescription medications may be used, such as pain medications, anti-anxiety medications, muscle relaxants, and anticonvulsants. There are also numerous alternative treatment options available such as compression therapy, warm/cold baths, tonic water, oral magnesium, and electric nerve stimulation.

Will my Restless Leg Syndrome (RLS) get worse over time?
Symptoms of Restless Leg Syndrome (RLS) are known to worsen over time. While many experience periods of symptom-free remission, RLS typically re-emerges at some point. Left untreated, RLS symptoms can both worsen and cause other conditions, such as daytime fatigue, depression, travel complications, memory and concentration impairment, insomnia, and exhaustion.
How is Restless Leg Syndrome (RLS) diagnosed?
The National Institutes of Health (NIH) established five specific criteria that must be met for a diagnosis of RLS:
- An overwhelming urge to move the legs, often associated with other unpleasant, uncomfortable, or abnormal sensations.
- The urge to move the legs begins or worsens during periods of rest or inactivity.
- The urge to more the legs is temporarily, partially, or totally relieved by leg movements.
- The urge to move the legs begins or worsens in the evening or night.
- The above symptoms are not due to any other behavioral or medical condition.
For more information about Restless Legs Syndrome and treatment options contact The New Jersey Vein and Vascular Center today!
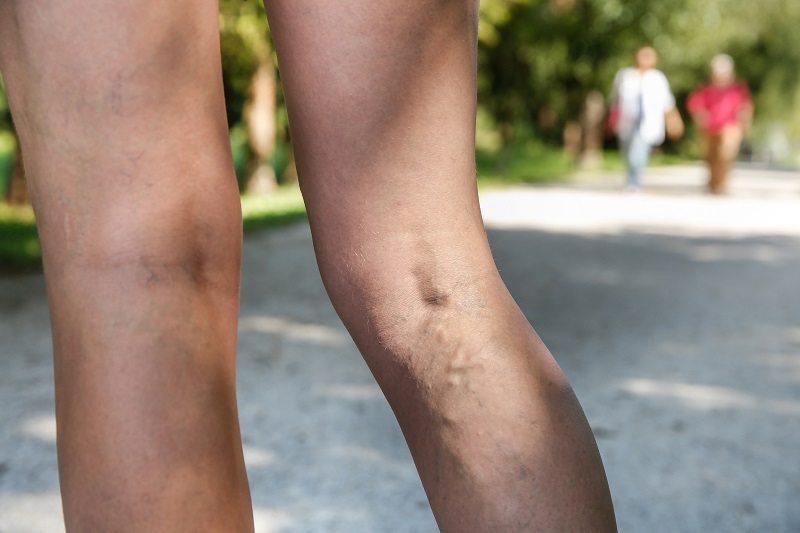
Jun 29, 2017 | News
A mainly sedentary lifestyle can contribute to the pain and appearance of varicose veins. One of the best ways to improve them is to participate in an exercise program that improves circulation without putting too much stress on your legs and helps with maintaining a healthy weight. Sports and exercising prevent varicose veins so get up and start moving.

Do get out and walk! Walking is probably one of the most important and recommended exercise for varicose vein sufferers, as it is fairly gentle on your legs while promoting circulation. So instead of just grabbing the mail, walk around the block and get your body moving!

Don’t jog or run on hard surfaces. The literal “pounding the pavement” can stress the legs, causing swelling of varicose veins. Instead, try a gentle jog on an even, softer surface such as grass.

Do get in the water! Swimming is a great low-impact exercise that can further develop your calf muscles and aid in improving circulation. This exercise can be done at any level and is great for summer fun.

Don’t participate in high-impact exercise. Heavy weightlifting, while a great workout, can be dangerous for a varicose vein sufferer, as it can put too much strain on the veins of your legs. Using lighter weights with fewer repetitions may be an option if weightlifting is something you love to do. Other such exercises include squats, lunges, and even yoga. Any exercise that increases abdominal pressure can increase leg vein pressure, leading to pain and swelling of varicose veins.

Do get out and bike! Cycling, like walking and swimming, is an ideal low-impact activity that improves circulation while building and strengthening leg muscles. Take a family bike ride in your neighborhood or bring your bike to the park to see more wildlife.

Don’t participate in contact sports. In sports such as football, rugby, and even tennis and skiing. The high probability of injury and sudden, quick movement can be counterproductive to leg vein health.

Starting with walking, cycling, or swimming for 30 minutes a day is a great way to alleviate the pain and appearance of varicose veins.
For more information about your vascular health, contact NJVVC today!


































