Did you know knee replacement surgery or treatment of other orthopedic injuries can significantly affect vein health? Or that sometimes, varicose vein problems can be the actual cause of knee pain?
Here’s information about orthopedic surgery and varicose veins—what you need to know.
CVI, Varicose Veins, DVT, and Orthopedic Surgery
First, a few definitions to help clarify our discussion.
Chronic Venous Insufficiency (CVI)
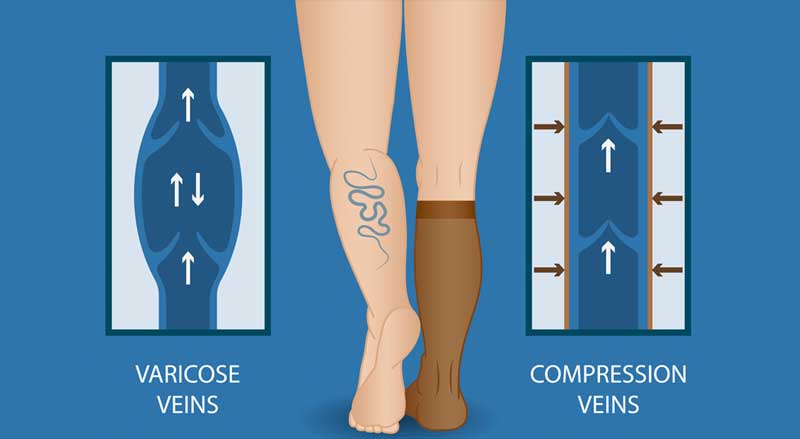
Chronic venous insufficiency (CVI) is a medical condition where damaged veins in the leg are unable to pump blood in the proper direction—to the heart. Blood pools in the veins. The veins become large and are called varicose veins.
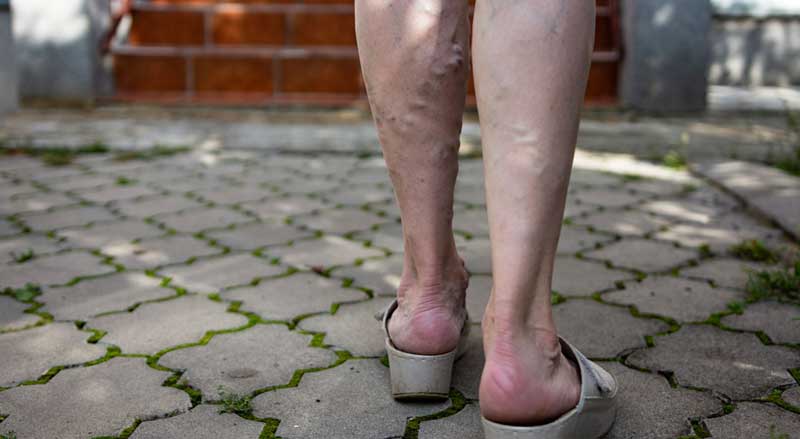
Varicose Veins
Varicose veins, often occurring in the legs, usually bulge just below the skin’s surface. They look twisted and enlarged and can be blue, red, or skin colored.
Common symptoms of varicose veins in the leg include:
- Pain or discomfort
- Swelling
- Aching and heaviness
- Itchiness
Deep Vein Thrombosis (DVT)
DVT is a common and serious cause of chronic venous insufficiency. With DVT, a blood clot has formed and damaged the valve in the vein.
A person is more at risk for DVT if they are older, obese, smoke, have a family history, or take certain medications.
Signs of deep vein thrombosis include:
- Persistent pain in leg
- Warm, red, tender skin
- Swelling of the calf, ankle, foot, or thigh
Deep vein thrombosis can become life-threatening if a blood clot breaks off and travels to the lungs.
Orthopedic Surgery
Orthopedic surgery is surgery performed on:
- Bones
- Muscles
- Ligaments
- Tendons
- Joints
Orthopedic Surgery Can Cause Vascular Problems
Orthopedic surgery, such as knee replacement or hip surgery, carries a risk of causing DVT.
Thankfully, there is now technology that makes it easy for a vein specialist to determine if a person is experiencing vein problems. And there are effective treatments for these problems, including DVT.
It’s very important that post-surgical patients remain vigilant about this possibility and contact their doctor if they experience signs of DVT.
It’s good to know that most DVT occurrences in the veins of the calf usually go away on their own without medical intervention. However, this reassuring fact doesn’t mean you should ever ignore any DVT signs you’re experiencing.
At NJVVC, our patients benefit from the most modern technology available for diagnosing and treating vein problems.
Watch and listen to our varicose veins specialist, Dr. Stuart Miller, as he explains the signs, symptoms, and treatment of varicose veins and other vein problems.
https://www.youtube.com/watch?v=wHu_hxT7o-Y&t=85s
Have Leg Veins Assessed Before Knee Replacement Surgery
If you have been told you need knee replacement surgery, knee arthroscopy, or hip replacement surgery, first visit a vein specialist. There are several important reasons why.
The Problem May Be in Your Veins!
Sometimes, the cause of knee pain is actually venous insufficiency. And only vein treatment will correct this—not knee surgery.
Vein Treatment Will Improve Your Post-Surgical Recovery
Many patients experience knee joint arthritis and venous insufficiency at the same time. This is because these two conditions most often occur in older adults.
If you have both arthritis and venous insufficiency, be sure to address your vein problems first. It will help with your post-operative recovery in these ways:
- You’ll have a greatly reduced chance of developing DVT
- There will be less swelling of the leg
- The surgical wound will heal better
Sometimes, treatment by a varicose vein treatment doctor is so effective in relieving knee pain that surgery can be put off for a while or even be cancelled altogether.
It’s always a good idea to first opt for this less invasive treatment before undergoing invasive knee surgery.
A comprehensive vein evaluation by our vascular specialist is completely non-invasive and non-painful.
Prior Orthopedic Injuries
Have you had a prior orthopedic injury such as a broken leg or ankle sprain? If so, you may be more likely to develop varicose veins later in life if you already have several other risk factors, including:
- Sitting or standing for long times each day
- A family history of varicose veins
- Older age
- Are female
- Are overweight
All orthopedic injuries in the leg won’t necessarily cause you to develop varicose veins later, but they do increase the risk.
Why Orthopedic Injury/Surgery Can Cause Varicose Veins
There are several ways an orthopedic injury or surgery can contribute to varicose vein development, including:
- A cast or recovery results in long immobilization of an area of the leg
- Altering how you put pressure on a leg or foot can, over time, add additional pressure on specific veins in the same or other leg
Sometimes, if you have a leg injury along with a predisposition to varicose veins, it shortens the time before varicose veins first appear.
How to Reduce Your Risk of Varicose Veins After Orthopedic Surgery
There are ways to reduce your long-term risk of varicose veins even after an injury or surgery.
They are:
- Keep your weight at a healthy level
- Stay active and avoid sitting for prolong periods of time
- Wear compression socks to help blood circulation
Tourniquets in Orthopedic Surgery
Surgeons use a tourniquet in orthopedic surgery to reduce blood loss and create a clearer area for the orthopedic surgeon to operate on.
The NIH has reported that using a tourniquet in orthopedic surgery on the lower extremities increases the incidence of deep venous thrombosis. It calls for further study and minimized non-necessary tourniquet use in surgery on high-risk patients.